|
SIX ARGUMENTS FOR A GREENER DIET

Following is a synopsis of Six Arguments for a Greener Diet, the Center for Science in the Public Interest’s latest book, which explains why eating fewer animal and more plant foods protects our health, planet and livestock. In keeping with CECHE’s stated mission, the synopsis focuses on human health concerns and recommendations raised in the book, and how environmental and animal welfare issues relate to them. Americans consume more than 1 billion pounds and 1 trillion calories of food every day. And while research and a host of organizations, including the Center for Science in the Public Interest (CSPI), the Center for Communications, Health and the Environment (CECHE) and the federal government, tout the benefits of a diet high in fruits, vegetables and whole grains, the typical American diet remains animal-rich and health-poor. According to recent reports by CSPI, the United States Department of Agriculture (USDA), the American Cancer Society and other reputable sources, the current American diet is linked to a high risk of health problems, including, but not limited to, heart disease, stroke, cancer, diabetes and obesity. In addition, producing animal foods to support our present eating pattern consumes more energy, fertilizer, pesticides, water and land, and generates more pollution and greenhouse gases than growing plant foods. These environmental effects further undermine human health, and underline how dietary decisions reverberate throughout our bodies, and the world. The Current American Diet And Its Health Consequences Americans are eating more flesh foods, including beef, pork, chicken, turkey and seafood. In 2003, we ate more of each of these foods than we did a half-century earlier, with the biggest increase for poultry. Although we are consuming one-third fewer eggs than in 1953, we are eating four times as much cheese, which is high in saturated fat and a greater promoter of heart disease than the dietary cholesterol in eggs. 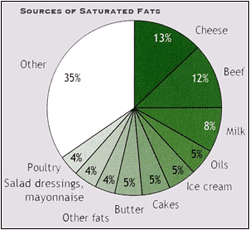
Americans are also consuming massive amounts of refined grains (white bread, pasta and rice), soft drinks, baked goods, fried foods and salt. And while the average American eats 11 servings of grains daily, only one of those servings is whole grain. At the same time, one-third of the vegetables we eat are iceberg lettuce and potatoes, two of the least nutritious, and we are consuming only one-third the recommended amount of the most nutritious vegetables (deep yellow and dark leafy green vegetables, and beans), according to the USDA. Poor Diet Linked to Disease and Untimely Death At least one of every six deaths in the United States upwards of 340,000 each year is linked to a poor diet and sedentary lifestyle, according to a 2004 study in the Journal of the American Medical Association. In fact, the average American is about as likely to die from a disease related to diet and physical inactivity as from smoking tobacco and far likelier to die from diet and inactivity than from an automobile accident, homicide or infectious disease, concluded the 2002 National Vital Statistics Report. Ultimately, a diet rich in fatty animal products and poor in whole grains, fruits and vegetables consumes the consumer, resulting in higher rates of heart disease, stroke, certain cancers, diabetes and obesity that cause hundreds of thousands of premature deaths each year. In all, animal foods may be responsible for 50,000 to 100,000 of these untimely deaths. Probably the biggest health benefit from eating less animal products (except fish) is a lower risk of heart disease. While vegetables, fruits and whole grains protect against heart disease, red meat, which often contains large amounts of saturated fat and cholesterol, does not. Even small amounts of saturated fat a totally unnecessary dietary addition increase the risk of heart disease. And our bodies already produce all the cholesterol they need, so adding more from animal products (the only place cholesterol occurs) simply elevates low-density (LDL) blood cholesterol levels, and the risk of heart disease. According to the American Cancer Society and a host of research projects, red meat may also increase the risk of cancer of the colon and rectum. A 2002 meta-analysis indicated a 35 percent increased risk of colon cancer in people who ate red meat and a 31 percent increase in people who ate processed meat compared to those who ate little or no meat. And a systematic review of cohort studies on the subject found that every 3.5-ounce-per-day increase in red meat consumption was associated with about a 15 percent increased risk of colon cancer, while every 1-ounce increase in daily consumption of processed meat was associated with an almost 49 percent higher risk. New research suggests that processed red meat in particular also increases the risk of pancreatic cancer and diabetes. Poultry does not appear to contribute directly to chronic disease unless deep-fried in partially hydrogenated oil. Diet-Related Environmental Risks Compound Human Health Problems With its reliance on fuel, fertilizers, pesticides and, of course, livestock, an animal-rich diet takes an environmental toll, polluting the planet, animals, and ultimately, humans. Meat, full-fat dairy products and fatty fish tend to be the major food sources of environmental contaminants, including pesticides, industrial chemicals and various pollutants, all of which often accumulate, and persist for many years, in animal fat. Some studies on farmers who regularly apply pesticides suggest significant human health risks associated with them, including higher rates of prostate cancer, melanoma, and Hodgkin’s and non-Hodgkin’s lymphoma. While most consumers are concerned about residues on fruits and vegetables, fat-soluble pesticides in animal products actually pose the bigger health threat because livestock are fed large quantities of pesticide-tainted feed grains and accumulate pesticide residues in their fat. Meanwhile, the USDA estimates that 5 percent of agricultural pesticides are washed away from farmland, threatening the safety of drinking water in many regions like California’s heavily farmed San Joaquin-Tulare Basin, where at least one pesticide was found in 59 percent of samples taken from groundwater wells. According to the federal Centers for Disease Control and Prevention, pathogens in food cause about 76 million illnesses, 325,000 hospitalizations and 5,200 deaths each year, and generate at least $6.9 billion annually in medical and related costs. According to a CSPI database of U.S. outbreaks linked to microbial hazards, almost 60 percent were associated with animal products or germs normally associated with livestock. In the recent Salinas Valley spinach contamination, flooding may have resulted in feces-contaminated runoff to bring the bacteria into contact with the produce. Meanwhile, the federal government’s current food-safety system is incomplete and fragmented, allowing neither for the tracking of animals and meat from the farm to the table, nor the recall of suspected food products. And while the USDA inspects meat and poultry plants daily, the Food and Drug Administration (FDA) inspects other operations an average of about once every five years. Pollution and the Factory Farm Between 1950 and 2003, red meat production more than doubled to 47 billion pounds per year and chicken production skyrocketed more than 20-fold to 41 billion pounds annually, while the number of farms dropped by 63 percent to 2.1 million. Consequently, today’s food industry relies on large-scale, densely packed production facilities to meet consumer demands. In addition to a host of animal welfare issues, these factory farms generate air pollution in the form of noxious odors, toxic gases and particulate matter. In fact, the feces and urine from today’s vast herds and flocks account for the Earth’s largest source of ammonia discharges. Meanwhile, potentially toxic pesticides from these facilities get blown far and wide to the tune of 40 to 60 percent applied to crops reaching the Earth’s atmosphere, according to the USDA. And the extensive herds of cattle release great volumes of the greenhouse gas methane, which, on a pound-for-pound basis, is 23 times more conducive to global warming than carbon dioxide, and at concentrations of 5 to 15 percent (often reached in manure storage tanks), can asphyxiate people, causing occasional deaths among farm-workers every year. The Science Behind Eating Green(er) While animal products do not have a monopoly on causing harm, six solid arguments for pursuing a green, or at least a greener, diet include:
Are Vegetarians Healthier? Research shows that the average vegetarian is healthier than the average carnivore. According to CSPI’s scientifically generated estimates, avoiding animal fats would annually save about 63,000 lives (+/- 25,000 because the estimate is based on inexact assumptions) and about $100 billion. (See Figure 1.) 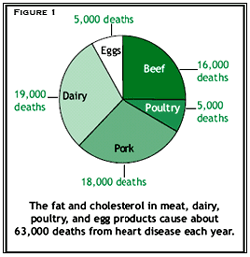
About half of American Seventh-day Adventists (SDAs) follow a vegetarian diet or eat meat less than once a week, and on average, SDAs (whose religion advocates abstinence from meat, poultry, alcohol and tobacco) consume less saturated fat and cholesterol, and more dietary fiber than the average American. Studies reveal that vegetarian SDA women and men live 2.5 and 3.2 years longer respectively than their non-vegetarian counterparts. Non-vegetarian SDA men also have twice the rate of fatal heart attacks as vegetarian SDA men, and hypertension is twice as common in non-vegetarian SDAs as in vegetarian. Diabetes is also twice as common in non-vegetarian SDAs as in vegetarian. Meanwhile, prostate cancer is 54 and colon cancer is 88 percent more common in non-vegetarian than in vegetarian SDAs. Studies of non-SDA vegetarians yield similar results, revealing that vegetarians enjoy lower risks of major chronic diseases and live longer (and generally healthier) lives than non-vegetarians. In fact, vegetarian diets may actually help reverse and treat chronic diseases. Prescribing a very low-fat vegetarian diet, moderate aerobic exercise, smoking cessation and stress reduction to patients with moderate to severe heart disease, Dean Ornish of the University of California in San Francisco and his colleagues not only saw improved cholesterol levels and significant weight loss, but the unclogging of arteries, and the prevention of angina and heart attacks. Lipid-lowering statin drugs were not needed; and the lifestyle changes alone were as effective as coronary bypass surgery in reducing angina. Low-fat vegetarian diets can also treat type 2 diabetes. How Much Risk Can Be Cut With a Plant-Based Diet? Several studies have found that men and women who consume the most fruits and vegetables have the lowest levels of LDL (bad) cholesterol and a reduced incidence of heart disease – generally 5 to 30 percent lower – than those consuming the smallest amounts. Meta-analyses found that each additional serving of fruit or vegetable per day was associated with a 16 percent lower mortality from heart disease and that each additional serving of fruit was associated with an 11 percent decrease in the risk of stroke, with vegetables having a similar effect. Fruits and vegetables also appear to play a modest role in cancer prevention, especially of the mouth, esophagus and stomach. And tomatoes, citrus fruits and cruciferous vegetables may protect against prostate, lung and bladder cancer respectively. Eating whole grains also appears to reduce the risk of heart disease and stroke. In a meta-analysis of 13 epidemiology studies, James W. Anderson of the Metabolic Research Center at the University of Kentucky concluded that people who ate the most whole grains had a 29 percent lower risk for heart disease than those who ate the least. In addition, eating more whole grains was associated with a one-third lower risk of ischemic stroke. Whole grains may also protect against diabetes, according to three large epidemiology studies that found about a 25 percent lower risk of diabetes for people who ate the most whole grains. Several studies strongly suggest that nuts (including peanuts, which account for two-thirds of Americans’ nut consumption and are technically legumes) also protect against heart disease. In one study, individuals who ate nuts one to four times a week had a 22 percent lower risk of heart attack than those eating nuts less than once a week. And eating nuts five or more times per week was associated with a 51 percent lower risk, with results consistent in men and women, and in younger and older people. While not plant-based, fish, like fruits and vegetables, also reduces the risk of heart disease: A 2004 meta-analysis found that individuals who ate fish five or more times per week had an almost 40 percent lower risk of dying from coronary heart disease. Fish consumption may also prevent strokes and protect against colorectal and prostate cancer. Contaminants such as PCBs, mercury and dioxins may undermine fish’s overall healthfulness, but for the average adult, the cardiovascular benefit from the omega-3 fatty acids in farmed salmon, for instance, far outweighs the cancer risk from PCBs. CSPI estimates that if 100,000 people ate one serving of farmed salmon per week, one person would develop cancer, but 1,500 people would be spared death from cardiac arrest. Fiber, especially soluble fiber and fiber from grain products, has also been linked to a lower risk of heart disease, and all minimally processed plant-based foods contain it (unlike animal products, which contain no fiber at all). Meanwhile, most fats and oils in plants contain beneficial mono- and polyunsaturated fatty acids that lower the bad cholesterol in blood. According to a Harvard study of more than 80,000 women, researchers estimated that substituting unsaturated fat for about one-third of the saturated fat in a typical diet would reduce the risk of heart disease by a hefty 42 percent. Although still in the early stages of research, phytochemicals, which are naturally present in plants, may assist with disease prevention. What Does It Mean To Eat Green? What Dietary Changes Are Needed? Not everyone will choose to be a vegetarian. But even modest changes – like eating a prudent diet (one with higher intakes of fruit, vegetables, legumes, whole grains, fish and poultry) – can yield life-saving results, reducing the risk of heart disease by 30 percent or more, according to two prominent studies. Today’s basic dietary message is clear and involves three steps recommended across the board by health organizations: (1) Base your diet largely on vegetables, fruits, beans, whole grains and healthy oils; (2) Eat fish and only modest amounts (if you choose to eat them at all) of fat-free or low-fat meat and dairy products; and (3) Cut way back on salt, refined sugars, white flour and partially hydrogenated oils. Published by the USDA and U.S. Department of Health and Human Services, the 2005 Dietary Guidelines for Americans (http://www.healthierus.gov/dietaryguidelines/) generally recommends daily intake of: 6-8 servings of grains, predominantly whole; 4-5 servings of vegetables, especially dark leafy green and orange ones, and beans and peas; 4-5 servings of fruit; 2-3 servings of fat-free or low-fat milk and equivalent milk products; two or less servings of lean meats, poultry and fish; and 4-5 servings of nuts, seeds and legumes. It also limits sodium consumption to 2,300 milligrams (mg) per day, and states that people with high blood pressure, African-Americans and people who are middle-aged or older should limit themselves to 1,500 mg. Two healthy diets that are easy to follow are the modified Dietary Approaches to Stop Hypertension (DASH) Eating Plan and the Mediterranean Food Pyramid. Developed by the National Institutes of Health, the DASH diet emphasizes the intake of plant-based foods and severely limits salt intake. Repeatedly shown to lower blood cholesterol, blood pressure and the risk of cardiovascular disease, it calls for: 8-10 servings per day of vegetables; 7-8 servings of grains (preferably whole); 2-3 servings of low-fat dairy; 0-2 servings of seafood, poultry and lean meat; one serving of beans, nuts and seeds; 2-3 servings of oils, salad dressing and mayo; and no more than five servings of sweets per week. 
Based on the diet once consumed widely in southern Europe, the Mediterranean Food Pyramid includes modest amounts of dairy foods, fish, poultry and eggs, plenty of fruits, vegetables, beans and whole grains, and wine in moderation. It allows red meat only rarely. Both the DASH and Mediterranean diets specify much less refined sugars than most Americans eat and pretty much exclude butter and stick margarine. Meanwhile, for those who have concerns about eating animal products or about animal welfare, vegetarian or vegan diets can be exceedingly healthy and rewarding, and the American Dietetic Association and the Dietitians of Canada have produced a Vegetarian Food Pyramid as a guide. 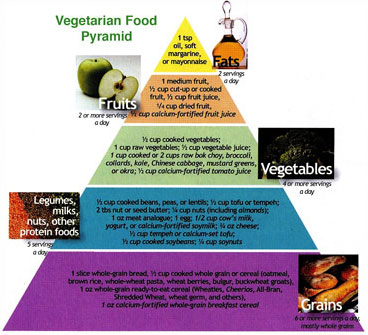
To encourage and support dietary change, CSPI created a Diet Scorecard that enables consumers to gauge the overall impact of their diet on their health, the environment and animal welfare (http://www.cspinet.org/EatingGreen/score.html). The organization also has an Eating Green calculator, which allows consumers to quickly compute the health and environmental effects of their current food intake and/or future dietary decisions (http://www.cspinet.org/EatingGreen/calculator.html). Even if you’re not ready for a big dietary shift, making several little changes quickly adds up to an overall healthier diet and cleaner environment – that could result in a longer-living you. For example, replacing one 3.5-ounce serving of beef, one egg and a 1-ounce serving of cheese each day with a mix of vegetables, fruit, beans and whole grains would:
Meanwhile, switching from a typical to a low-meat diet uses 41 percent less energy, and generates 37 percent less greenhouse gases and 50 percent less equivalents of respiratory irritant and acid rain-causing sulfur dioxide. Multiply such changes by millions of people, and it’s easy to see the dramatic improvements that dietary modification could achieve. Even without cutting back on beef and dairy foods, just shifting the cattle industry away from feedlots and toward leaner grass-fed beef and getting the dairy industry to cut the saturated-fat content of milk would yield big health, environmental and animal-welfare dividends. What Policy And Implementation Changes Are Needed, And To What End? Despite the well-recognized benefits of diets higher in plant-based foods and lower in animal products, relatively few people will change their diets (and few farmers will alter their growing practices) without encouragement from new government policies. Ideas to increase fruit and vegetable consumption include: earmarking $150 million per year (30 times the amount currently spent on the “5 A Day” program) for media campaigns to encourage people to make healthier food choices; expanding the highly successful Fruit and Vegetable Snack Program, which provides a free daily serving of a fruit or vegetable to schoolchildren; providing bonus stamps for the purchase of fresh, frozen, canned or dried fruits and vegetables in the federal Food Stamp program; and providing more fresh fruits and vegetables, and less cheese, milk and eggs in the government’s Women, Infants and Children program. Meanwhile, levying a tax on higher-fat cattle, paying farmers more to deliver lower-fat milk and lowering the fat limit for ground beef and hot-dogs, and halving it for pork sausages, could help reduce the fat content of meat and milk. And consumers might be swayed to make healthier decisions by a new labeling system that rates foods according to their healthiness. They might also choose more wisely if chain restaurants and fast food outlets were required to list the calorie, saturated and trans fat, and sodium content of each food item on their menus and menu boards. To help prevent foodborne diseases, the federal government should upgrade food-safety measures and consolidate the health and food-safety responsibilities of the USDA, FDA and other federal groups into a single independent agency. It should also stop supporting ads that promote milk, beef and eggs, while providing more healthful meals in its own government-run facilities. Beyond that, government could ensure that the price of meat reflects the costs of heart disease and the air and water pollution from factory farms. With regard to such food-processing environments, federal and state governments should limit the density and total number of animals at these facilities, which, in conjunction with aggressive enforcement of the Clean Air Act, Superfund and Community Right-to-Know laws, would help prevent air and water pollution. By mounting intensive programs and providing loans, grants or tax breaks, the USDA and state departments of agriculture could encourage a move away from pesticides and chemical fertilizers towards more organic methods or biotechnology; they could also tax fertilizers and pesticides to internalize some of their environmental costs and curtail their use. Reducing the amount of grain in cattle feed and the length of time cattle eat such feed, and developing a labeling system to identify meat, poultry and milk produced in an environmentally friendly and humane manner would help reduce greenhouse gases, while delivering healthier products. Research (and its support) also plays an important role in catalyzing change by providing insights on the effects of different diets and farming methods, and suggesting ways to improve national policies and industry practices. In addition to government actions, progressive companies and farmers can help turn the tide. Some already are – voluntarily producing healthier, more humane foods, and minimizing their impact on the environment. If only “some” would become that all-important “many.” With the recent food scares (including the very recent Salmonella outbreak and the October lettuce, carrot juice and ground beef recalls), the ensuing media coverage, and the American consumer’s increasing willingness to spend more for organic foods, perhaps “many” is already in the making. Click here to read Q&A with the author of Six Arguments For A Greener Diet |
|
|||||||||||
Questions? Comments? Concerns? E-mail CECHE at CECHE@comcast.net Go back to the CECHE home page Go back to the CECHE home page
|

