Center for Communications, Health and the Environment

Eat Safe: Sweeping Policy Reforms, Surveillance and New Strategies Combat Global Outbreaks of Foodborne Illness
Once upon a time – within the last century, as a matter of fact – people grew their own food or got it directly from someone they knew. Populations ate locally; and foodborne illnesses and outbreaks were limited and contained.
 |
Today's global marketplace raises questions about both food source and food safety. |
Today, this close relationship with our most critical consumable is practically defunct. Food production is an international business, powered by multi-national corporations and peppered with products from faraway lands. Populations eat globally – shrimp from Vietnam, kiwis from New Zealand, papayas from Mexico – and foodborne outbreaks and illnesses (generally defined as infectious or toxic diseases caused by agents entering the body through the ingestion of food) are widespread and rampant.
Legislation is critical for food safety and defense, but it’s not enough. Many countries, companies and organizations realize this and are actively addressing the challenges and public health issues generated by today’s complex consumption environment.
This article highlights the many ways – evaluative, regulatory and cooperative – in which groups and governments around the globe are advancing the food safety imperative, including:
- national surveillance
- global initiatives
- unprecedented, comprehensive legislation
- self-policing programs
- multi-national partnerships, and
- national, regional and international food-safety symposia.
Food Fight
The actual global impact and costs of foodborne diseases are unknown, but experts, including those at the World Health Organization (WHO) and the U.S. Department of Health and Human Services (HHS), generally agree that such infections and outbreaks are preventable public health burdens.
 |
Cholera outbreaks have had devastating effects in both Latin America and Africa. |
Developing countries tend to suffer a larger share of foodborne illnesses due to the wide range of possible agents, including parasites, while the prevalence of diarrheal diseases in many of these countries suggests significant and deeply rooted food safety issues. In the aftermath of the Rwanda crisis in 1994, for example, cholera outbreaks resulted in at least 48,000 cases and 23,800 deaths within one month in the refugee camps in Goma, the Congo, WHO reported. And WHO, the U.S. Centers for Disease Control and Prevention (CDC) and various other sources note that the re-emergence of cholera in Peru in 1991 led to more than 1 million cases and 9,600 deaths across Latin America (which had been cholera-free for more than a century), and cost Peru US $770 million due to sharp drops in food exports and tourism. Meanwhile, according to a 2007 WHO fact sheet (N°237), the percentage of the population suffering from foodborne diseases each year in industrialized countries has been reported to be up to 30 percent, and diseases caused by the major pathogens, including Salmonella and certain strains of E. coli, are estimated to cost up to US $35 billion annually (1997 figures) in medical costs and lost productivity in the United States alone.
“About 48 million people (1 in 6 Americans) get sick, 128,000 are hospitalized, and 3,000 die each year from foodborne diseases,” reports the CDC in its “2011 Estimates of Foodborne Illness In the United States.” And with American food imports nearly doubling between 1998 and 2007, from $41 billion to $78 billion, according to a March 2012 U.S. Department of Agriculture (USDA) Economic Research Service (ERS) report, concern over food illnesses and outbreaks remains high.
 |
Food imports are increasingly common, and difficult to monitor. Source: U.S. Navy photo by Mass Communication Specialist Seaman Leah C. Allen (RELEASED); Wikimedia Commons |
ERS estimates that, today, about 16 percent of all food eaten in the United States is from other countries, with as much as 85 percent of all seafood and 60 percent of fresh produce in certain seasons imported. Meanwhile, “... the F.D.A. inspects less than one pound in a million of imported foods,” remarked a June 17, 2012 New York Times article on the subject.
“[I]mported foods mean we depend on the food safety systems of other countries,” emphasize Medscape’s Janet Kim and CDC deputy director, Division of Foodborne, Waterborne and Environmental Diseases, Robert V. Tauxe, in a Medscape News slideshow entitled “The Major Foodborne Illness Outbreaks of 2011.”
With the world’s food sources and sourcing so intertwined, an unidentified strain of Salmonella in sushi tuna produced in an unmonitored, unhygienic facility can end up sickening people halfway across the world – and it has. In fact, from 2005 to 2010, 39 U.S. outbreaks and 2,348 illnesses were linked to imported food, particularly fish and peppers, from 15 countries, the CDC reports. Of those outbreaks, almost half (17) occurred in 2009 and 2010, and nearly 45 percent of the implicated foods came from Asia.
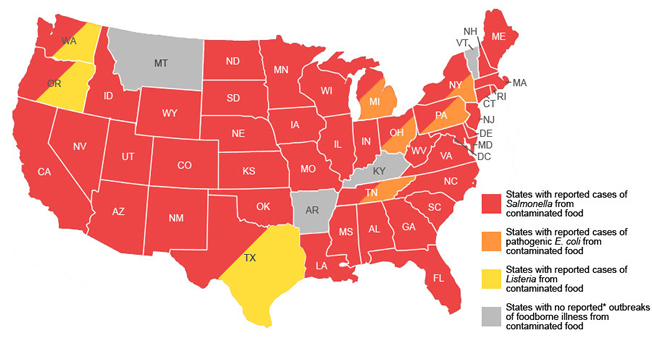 |
2010 Foodborne-Illness Outbreaks by Pathogen Linked to FDA-Regulated Foods Source: The Make Our Food Safe coalition |
“[I]f you have something which gets contaminated or infected in one country it can be in 50 countries or 100 countries or 200 countries," noted WHO Assistant Director-General Keiji Fukuda during a fall 2011 conference in Singapore on improving preparedness against global health threats, as reported by Agence France-Presse.
Recent Food Outbreaks and Their Impact
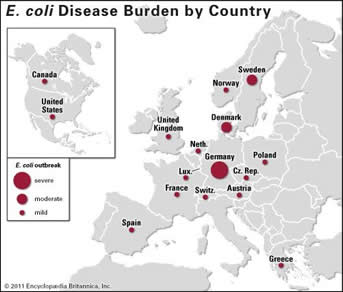 |
A 2011 outbreak of E.coli in Germany had far-reaching effects. |
In fact, the deadliest known worldwide food outbreak in recent history occurred in the spring of 2011. Caused by a new and unusually virulent strain of E.coli in locally produced raw sprouts, it first appeared in Germany, later surfaced in France and was ultimately tied to a single lot of fenugreek seeds from Egypt. The outbreak affected persons who travelled to Germany from 11 other countries in the European Union (EU), Norway and the United States, infecting almost 4,000 people, killing 51 across Europe and causing massive losses to vegetable farmers.
Later that same year, America suffered its deadliest case of foodborne illness since the 1920s. Fresh, whole cantaloupes from a Colorado farm were linked to a first-of-its-kind multi-state Listeria outbreak beginning in August and resulting in 146 people sickened, 142 hospitalized and 30 dead across 28 states.
While most foodborne diseases are infrequent and not reported, foodborne disease outbreaks may take on massive proportions, reminds a 2007 WHO fact sheet. For example, a 1994 outbreak of salmonellosis in the United States due to contaminated ice cream affected an estimated 224,000 persons nationwide, while a 1988 outbreak of hepatitis A, resulting from the consumption of contaminated clams, impacted some 300,000 individuals in China.
Thus far in 2012, the United States has suffered eight reported food outbreaks, down from 13 in 2011 and 18 in 2010. Among this year’s incidents are back-to-back Salmonella outbreaks that continue to reverberate: one, first identified in late August in Canada and linked to Mexican-grown mangoes, has sickened 127 people in 15 states; and the other, tied to cantaloupes from an Indiana farm, has killed three and sickened 261 in 24 states. Meanwhile, a May outbreak involving two strains of Salmonella in a frozen raw yellowfin tuna product imported from India by a California-based company caused more than 425 people from 28 states and the District of Columbia to become ill.
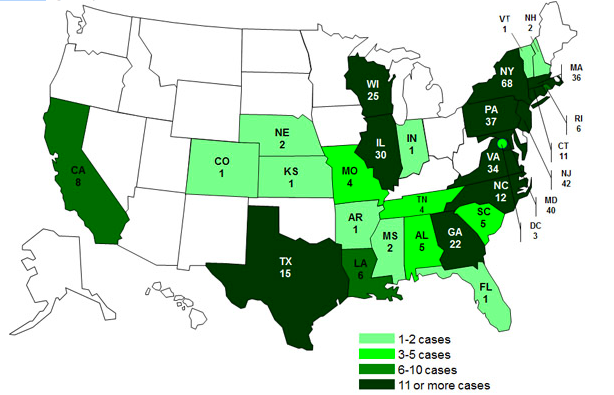 |
Case Count Map of Persons Infected with Two Strains of Salmonella Associated with a Raw Scraped Tuna Product, by State (As of July 25, 2012) Source: CDC |
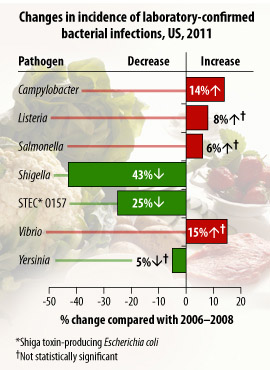 |
Source: CDC |
In general, while Salmonella appears to be having a heyday, and the incidence of Vibrio and Campylobacter infections has increased, the rate of foodborne illness in the United States has actually dropped by nearly a quarter since the late 1990s, according to the CDC’s most recent report on the subject. Released in June 2012, the group’s FoodNet 2011 report found that the overall incidence of six common foodborne pathogens – Campylobacter, Listeria, Salmonella, Shiga-toxin producing E. coli O157, Yersinia and Vibrio – was 24 percent lower in 2011 than in the years between 1996 and 1998. The rate of foodborne disease was no lower in 2011 than in 2006, however, and other germs that commonly cause foodborne illness, such as Norovirus, were not included in the data.
The CDC attributes this downward trend to a number of factors, including enhanced knowledge about preventing contamination and surveillance tools such as PulseNet, a network of public health and food regulatory agency laboratories that perform real-time molecular “fingerprinting” of foodborne disease-causing bacteria to facilitate the detection and investigation of multi-state (and multi-nation) outbreaks.
The Purpose and Power of Surveillance
The ability to classify, monitor and track foodstuffs and the pathogens related to them is a valuable weapon in the fight against foodborne illness and widespread outbreaks. In addition to PulseNet (above), the United States maintains the Foodborne Diseases Active Surveillance Network or FoodNet, a collaborative program launched in 1995 among the CDC, 10 state health departments, the USDA’s Food Safety and Inspection Service and the U.S. Food and Drug Administration (FDA). As referenced above, FoodNet reports on trends in foodborne infections and tracks the impact of food safety policies nationally by conducting active population-based surveillance for laboratory-confirmed cases of infection caused by any of seven bacteria and two parasites commonly transmitted through food. In 2011, FoodNet identified nearly 19,000 infections, according to the CDC.
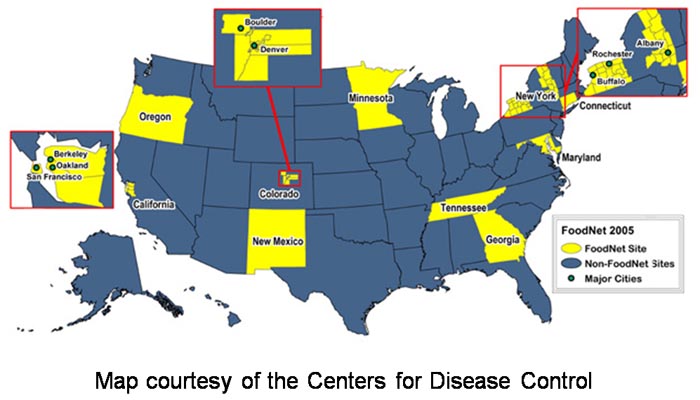
There’s also the Foodborne Disease Outbreak Surveillance System, which captures outbreak data on agents, foods and settings responsible for illness via reports submitted by state, local and territorial public health agencies through the National Outbreak Reporting System. For direct access to this data, the public can search the Foodborne Outbreak Online Database (FOOD) or turn to nongovernmental resources such as the Center for Science in the Public Interest’s Outbreak Alert! for current information and assessment of food recalls and developing cases such as the August and May 2012 Salmonella outbreaks, as well as the September 2012 Listeria (in ricotta cheese) and Salmonella (in peanut butter) incidents. Specific pathogens are also monitored via targeted programs like the Listeria Initiative, with their data linked to network databases such as PulseNet to aid in rapid case-control analyses and the investigation of clusters and outbreaks.
During the 2011 multi-state outbreak of listeriosis linked to whole cantaloupes, PulseNet public health laboratories rapidly identified the outbreak strains in Colorado patients, according to the CDC, and then connected them with illnesses in 25 other states, quickly identifying people who were part of the outbreak and showing that the same strains were present in the implicated cantaloupe, as well as the packing shed.
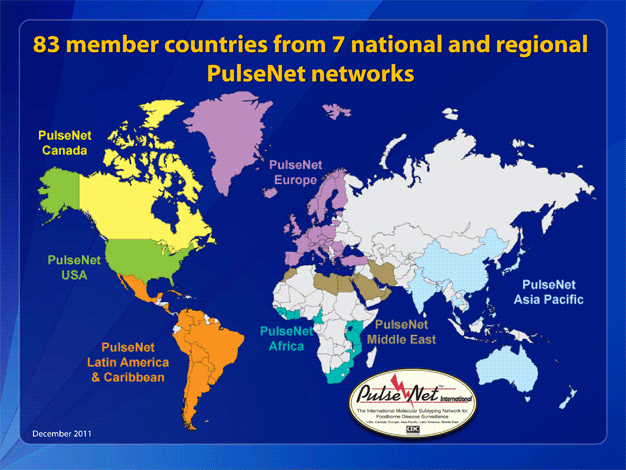
Systems like PulseNet enable authorities to know that illnesses in different states are part of the same outbreak, and that multiple states are affected. “Without PulseNet, many multi-state outbreaks would not be detected or controlled at all,” the CDC states. For example, the expansive 2009 U.S. outbreak of Salmonella infections linked to peanut butter (714 cases and six deaths in 46 states with more than 3,900 different tainted products recalled) “would not have been detected at all, and might have continued for months or years.”
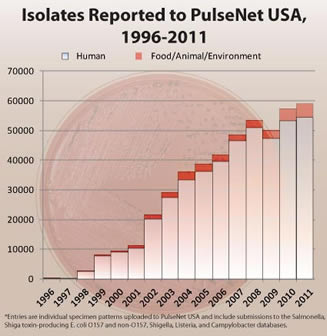 |
Source: CDC |
“PulseNet-triggered outbreak investigations” have led to the recall of more than half a billion pounds of contaminated food, according to the CDC, and “have highlighted unrecognized problems in food production and distribution industries, such as the beef, produce, tree nut, peanut, egg, and spice industries, ultimately resulting in major change to industrial processes and improved food safety.”
In fact, since its U.S. birth in 1996, PulseNet has become a global network with national and regional laboratory systems in Canada, Europe, Latin America, the Asia-Pacific region, and to a lesser extent, Africa and the Middle East. These systems use standardized genotyping methods and share information in real-time to provide early warnings on foodborne infections and outbreaks, and track, source and combat them worldwide. For example, the PulseNet database was instrumental in identifying and tackling the 2011 E.coli outbreak in Germany/Europe and pinpointing the strain, pattern and variants in a 2010 Vibrio cholerae outbreak in Haiti.
And valuable information continues to accrue. From 1996 to 2011, “individual annual human illness specimens (isolated pathogens from human samples submitted to laboratories by physicians)” to PulseNet USA alone increased more than 200-fold, the CDC reported. And specimens from food, the environment and other sources increased more than 800-fold.
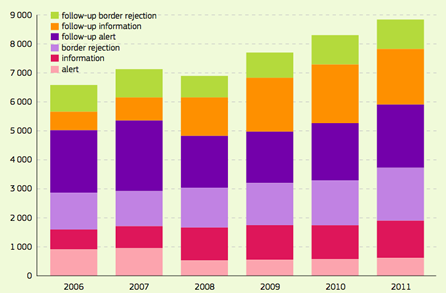 |
Evolution of the Number of Notifications to RASFF, by Notification Classification Source: RASFF 2011 Annual Report |
In addition to PulseNet, many countries operate independent surveillance networks. Established pre-Union in 1979, the EU’s Rapid Alert System for Food and Feed (RASFF) enables quick and effective exchange of information between member states and the commission when risks to human health are detected. According to the RASFF “Preliminary Annual Report 2011,” the system processed a record 3,730 original notifications, categorized as alert, information or border rejection, in 2011, an increase of 13 percent over 2010, when such notifications were slightly under 3,300. The most growth (17 percent) occurred in the area of border rejections, possibly due to a 2009 regulation which imposed stronger border controls on food of non-animal origin.
On a global level, WHO operates the Initiative to Estimate the Global Burden of Foodborne Diseases. Launched in September 2006 under WHO’s Global Strategy for Food Safety, the initiative aims to strengthen the scientific basis of food safety activities and assess and communicate foodborne risks. Its cornerstones are a Foodborne Disease Burden Epidemiology Reference Group (FERG), an expert advisory body tasked with assembling, appraising and reporting on global burden of foodborne disease estimates, and in-depth country studies designed to enable nations to conduct their own burden of foodborne disease assessments and policy context mapping. FERG is expected to release its estimates in December 2013, according to a report in WHO’s Food Safety News, No 44. Meanwhile, pilot country studies are underway in Albania, Japan, Thailand and Uganda to evaluate protocols and tools before commencing full country studies in WHO’s six regions.
WHO also maintains the Global Foodborne Infections Network, a program to detect, control and prevent disease throughout the food chain, and it produces a range of publications related to food safety.
Legislation and Food Safety
The real workhorses in the battle against foodborne illness are individual countries and the food safety legislation they enact and enforce.
Faced with increasingly intricate and immense food systems, many nations are reevaluating their food safety measures and instituting landmark changes in the name of public health, with the United States helping to lead the charge.
 |
Signed into law in January 2011, the FDA Food Safety Modernization Act is the most sweeping reform of U.S. food safety laws in more than seven decades. Source: modernsurvivalblog.com |
The most sweeping reform of U.S. food safety laws in more than 70 years was signed into law by President Barack Obama in January 2011. The FDA Food Safety Modernization Act (FSMA) focuses on preventing contamination, rather than reacting to it. The legislation addresses everything from preventive controls, and inspection and compliance to imported food safety, rapid response and productive food-protection partnerships, and it includes many firsts.
Under the law – and for the first time in history – the FDA has the authority to require comprehensive, prevention-based controls across the U.S. food supply. This translates into mandatory protective restrictions for food facilities as well as prescribed standards for the safe production and harvesting of fruits and vegetables.
The law also enables the FDA to hold food companies accountable for preventing contamination, and it enhances the agency’s ability to oversee and regulate imported foodstuffs. In fact, in an unprecedented directive, importers are now required to verify that the food products they are bringing into the United States are safe, and they must confirm that their suppliers are complying with “risk-based preventive controls” that provide the same level of public health protection as those required under FSMA. Food defense is also part of the equation, and FSMA gives the FDA the power to prevent intentional contamination and requires the agency to issue regulations to protect against the deliberate adulteration of food, especially at vulnerable points.
 |
|
The FDA can recall any and all contaminated or suspect food products.
Source: OpenCongress.com |
|
FSMA also imposes an inspection mandate that requires FDA checks to be based on risk and the frequency of inspections to increase at the nation’s more than 600,000 active registered domestic and foreign food facilities. Additionally, the law gives the FDA mandatory recall authority for all food products, and it directs the agency to build an integrated national food safety system in partnership with state and local authorities that will, among other things, improve training at all levels and provide grants related to food safety to eligible state, local, tribal, territorial and nonprofit entities.
To date, the FDA has issued two regulations under FSMA. These went into effect in July 2011, and they:
- Allow detention for up to 30 days of food products the agency believes have been produced under unsanitary or unsafe conditions, or are contaminated or misbranded (with no credible evidence required, as in the past).
- Require anyone importing food or feed into the United States to inform the FDA if any country has refused entry to the same product.
In enforcing these new rules, the FDA has detained various foods, including a cold-smoked ready-to-eat salmon product in February 2012 (inspectors later found Listeria monocytogenes within the food facility and on its processing equipment), and items at a food storage and processing facility in Washington state in October 2011, following an inspection that detailed widespread, active rodent and insect infestation.
FSMA also has resulted in the creation of targeted associations, including the Preventive Controls Alliance in 2011 and the Sprouts Safety Alliance in early 2012. Also under this legislative umbrella are two pilot projects to explore and demonstrate rapid, effective food tracking and tracing methods. The focus of the pilots are FDA-regulated foods involved in significant outbreaks in the five years preceding FSMA: tomatoes; frozen Kung Pao-style dishes that contain peanut products, red pepper spice and chicken; and jarred peanut butter and dry, packaged peanut/spice.
Most recently under the law, in June 2012, the FDA issued two grant solicitations related to emergency response/recall and inspections. In addition, it plans to provide up to $10 million to support manufactured and retail food program standards implementation, laboratory accreditation and increased participation in the Rapid Response Team project, an initiative launched in 2008 to develop integrated immediate response to food and feed emergencies via state-based teams nationwide.
Meanwhile, on June 7, 2012, the federal government of Canada took a stab at its own piece of sweeping legislation when it introduced the Safe Foods for Canadians Act, a bill calling for a tough new national food safety law with greater penalties for violators, more unified enforcement powers and an overhaul of the country's food inspection system.
 |
|
India is entering a new era of national food safety with its recent, far-reaching regulations. |
At the same time, India is trying to enforce a new food safety rule nationwide that requires all food sellers, including millions of street vendors and roadside food stalls, as well as all trucks and vehicles that transport food across the country, to get registered or licensed. The August 4, 2012 deadline was fixed under India’s Food Safety and Standards (Licensing and Registration of Food Businesses) Regulations 2011, and according to a July 24, 2012 article in India Today, requires food business operators “to fulfill many safety, hygiene and sanitary conditions,” complete several documents and pay a fee, or risk heavy fines or closure. (In 2009, a similar food safety law was passed in China, creating a food safety committee and requiring licensure for all food producers, caterers and retailers.)
Also this summer, the Codex Alimentarius Commission, an international food standards body created in 1963 and jointly run by the United Nations (UN) Food and Agriculture Organization (FAO) and WHO, agreed on new global regulations. Measures adopted included new food safety standards on seafood, melons, dried figs, melamine levels in liquid baby formula and food labeling. According to WHO, “Codex members cover 99 percent of the world’s population,” and Codex Alimentarius (Latin for “Book of Food) standards often serve as a basis for national legislation, while providing food safety benchmarks for international food trade.
Self-Regulation
In addition to legislation, self-policing is important, both by the food industry at various stages in the food system, such as production, storage, distribution and retail sales, and by individual consumers in their homes and immediate environments.
Historically, the front line of food safety has relied heavily on industry insiders, with possibly undue emphasis placed on HACCP (Hazard Analysis and Critical Control Points) prevention-based food safety plans to minimize foodborne risks in the production stage. Implemented under regulation in the United States, Europe, Canada, Australia and New Zealand, and a high-priority program under Codex Alimentarius, HACCP plans place more ownership of the responsibility to identify and control hazards, and document the effectiveness of the system on food processors than on government inspectors, according to FDA.
In the United States, HACCP plans are company-written and government-approved. In them, food processors identify potential risks (e.g., improper temperature control, poor employee hygiene), then implement and monitor ways to minimize or eliminate such risks. For the last decade at least, all U.S. seafood, juice, meat and poultry processors have had to develop and abide by HACCP plans; and with the advent of FSMA, all U.S. produce processors must also now follow suit. (Previously, produce companies were held to voluntary standards and couldn’t be penalized for poor safety practices.) Currently, HACCP plans are voluntary for U.S. dairy plants.
 |
Stricter government oversight may help make self-policing a more viable food safety option. Source: FDA |
Despite prevention-based plans and new policies, to date, the results of self-regulating for food safety are mixed. In fact, according to a July 2011 posting (updated September 2011) of The Huffington Post, “The times when self-policing has been seen as most effective have been those in which the strategy was seen as strictly supplementary to strong governmental regulation.”
FSMA certainly ups the self-policing ante. It could ultimately lead to better self-management and -enforcement of food-safety plans because companies that receive warning letters are now required to pay for follow-up inspections and the FDA is now able to shut down businesses with severely flawed food safety plans if the companies don’t correct problems. In short, the consequences of outstanding violations and non-compliance are becoming palpable – and profit-related – making self-policing more viable. And possibly not a moment too soon, since more than 70 percent of safety plan violations for U.S. seafood and juice processors alone remained unresolved after more than a year, revealed a News21 2011 “How Safe Is Your Food?” project analysis of FDA records from September 2009 to December 2010.
Meanwhile, companies involved in food storage, distribution and retail sales are also expanding their options for food-safety self-management. In February 2012, for example, Maricopa County, Ariz., unveiled an innovative program to promote food safety practices at area food businesses, especially grocery stores and restaurants. Known as “The Cutting Edge,” the voluntary food safety management program requires participants to establish standard operating policies and procedures, train staff in them and monitor results to minimize the incidence of risk factors between routine inspections and visits by county health inspectors. In addition to targeted programs, restaurants and food service companies can turn to specially designed products, such as N2N Global’s Quality & Food Safety Manager, to assist with food safety, compliance and quality throughout the food supply chain.
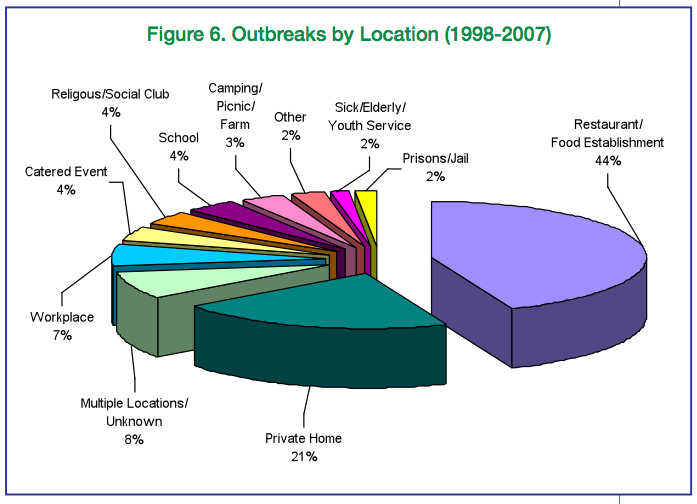 |
Source: CSPI, "All Over the Map: A 10-Year Review of State Outbreak Reporting" |
 |
|
Source: National Chicken Council and the Partnership for Food Safety Education |
For individuals, food safety seems decidedly more straightforward. It follows the same general guidelines as industry, but, with family health, and potentially lives, at stake and no profits on the line, self-policing actions like properly cleaning food, hands and food preparation areas, separating raw foods from ready-to-eat foods, keeping food properly chilled, and cooking foods to the proper temperature are often readily practiced.
Coming Together to Make a Difference
But for the world, going it alone isn’t an option. Given the international waterway of food product delivery and consumption, countries, corporations, their ministers, decision-makers and food service providers need to talk and work together to ensure the future of food safety, and the development of regulations and requirements that work.
The Codex Alimentarius Commission is a prime example of such cooperation. Its annual meeting is attended by 600 delegates representing 184 countries and the EU, and as noted above, is a launch point for new and updated international food safety standards and recommendations. In addition to developing “harmonized” global food guidelines and codes of practice to protect consumer health and ensure fair food trade, the Commission, which also has 208 observers, including 48 inter-governmental organizations, 144 nongovernmental organizations (NGOs) and 16 UN groups, promotes coordination of all food standards work by international governmental and nonprofit organizations.
 |
| The future of food safety depends on partnerships and cooperation developed through international groups like the Codex Alimentarius Commission and large-scale symposia.
Source: wordpress.com |
Large-scale symposia and conferences also help to grease the cooperative wheels. Held in Washington, D.C., in April 2012 and attended by 1,300 professionals from government, academia and the food industry, the 14th Annual Food Safety Summit spotlighted collaboration, specifically the teaming of industry and government to safeguard America’s food supply.
On the other side of the globe, in February 2012, more than 1,200 regional and international delegates dialogued on the future of food safety at the Seventh Dubai International Food Safety Conference. Organized in part by the International Association for Food Protection (IAFP), and its first Middle East symposium, the conference emphasized cooperation among regulatory agencies, health authorities and the food industry on issues such as foodborne disease surveillance, outbreak investigation and compliance. It also facilitated an open discussion between food control authorities in the Gulf Cooperation Council and representatives from the regional food manufacturing and trading sector.
The mission of the 3,600-member IAFP is to '”provide food safety professionals worldwide with a forum to exchange information on protecting the food supply.” For the past eight years, the organization’s European Symposium has provided a means for such an exchange with Europeans in industry, government and academia. IAFP is also a global partner of the China International Food Safety & Quality Conference, which brings together food safety professionals from across China and the world with global effect. Meanwhile, IAFP’s annual meeting is attended by more than 2,500 industry, academic and governmental food safety professionals from six continents and has become one of the world’s leading food safety conferences, as well as a unique opportunity for experts to liaise on current and emerging food safety issues, the latest science, and innovative solutions to new and recurring food safety problems.
Other organizations that actively advance collaboration and partnership include SELAMAT, a network organization that brings together stakeholders from Europe and Asia to share food production methodology, expertise, knowledge, best practices and policy developments with an emphasis on food safety, food quality and related issues such as food security, climate change and technology developments. Meaning “safety” in Malay and “safe” in Indonesian, SELAMAT, whose full project name is “Safety enhancement of edible products, legislation, analysis and management with ASEM (Asia-Europe Meeting) countries, by mutual training and research,” has been fostering cooperation, information exchange and sharing since 2004 via: workshops, flyers, lectures and publications; a network website (www.selamat.net); training courses; a Global Food Safety Legislation Portal and help desk; joint activities and research projects; and expert/specialist exchange between SELAMAT members.
Established in 2009 and based in Michigan, the Global Food Protection Institute (GFPI) is focused on protecting the world’s food supply through FDA-aligned training, new food protection technologies and inspired forums. Its International Food Protection Training Institute (IFPTI) provides intensive instruction in areas related to food safety and an opportunity for food manufacturers to learn side-by-side with local regulators, while its Emerging Technology Accelerator showcases cutting-edge food protection technologies and its Imagined Food Futures® Symposia convene experts and policymakers to tackle issues affecting global food protection. In September 2011, the GFPI received a $1.3 million grant from the FDA to aid in the implementation of the FSMA, specifically working to brief local regulators on the act and how to perform uniform inspections. In fact, the IFPTI was created to help develop normalized inspection standards and ensure that U.S. state and local regulators and inspectors apply these uniform rules.
Building stronger cooperative relationships with industry and counterpart agencies around the world is a hallmark of the FDA's “Beyond Our Borders” or “Globalization” initiative. The program supports worldwide harmonization initiatives, through which FDA and its partners develop common standards, and it facilitates agreements with foreign regulators that allow the FDA and its peers to share resources, knowledge and scientific expertise, and promote responsible international guidelines and regulations. Between 2004 and 2008, the number of such compacts more than doubled to 120 formal agreements with counterparts in 29 countries, the European Commission/EU and WHO, and it continues to grow. As of June 2012, the FDA had also signed 54 arrangements enabling the exchange of confidential information with foreign regulators in 23 countries, the EU and multilateral organizations, reported FDA Deputy Commissioner for Global Regulatory Operations and Policy Deborah M. Autor at the 116th Annual Association of Food and Drug Officials Education Conference.
To assist in developing closer working relationships and assembling global coalitions of regulators “dedicated to building and strengthening the product safety net around the world,” FDA is also establishing overseas offices in strategic locations. The first of these foreign offices opened in China in November 2008. (Around the same time, HHS signed legally binding, “precedent-setting” Memoranda of Agreements with China’s FDA counterparts to enhance the safety of food, feed and other items imported into the United States from China, boost technical cooperation between the agencies and foster the flow of information between regulatory systems.)
 |
Forging a closer working relationship with China is important to U.S. — and global — food safety. Source: conservativedailynews.com |
To date, the FDA has established 13 foreign posts, including three each in China, Latin America and Europe, two in India, one in Sub-Saharan Africa (in Pretoria, South Africa) and one in the Middle East and North Africa (in Amman, Jordan). The agency’s interactions with its counterparts in Canada, Australia and New Zealand are managed through its Rockville, Md., office, from where it also operates its Office of Harmonization and Multilateral Relations, which is responsible for coordinating and collaborating food and drug activities with various governments and international organizations, including WHO and the Codex Alimentarius Commission.
Conclusion
Foodborne illness is nothing new. What is different today is the complexity and rapidity with which such diseases can arise and spread across a country, continent or ocean, given a growing global menu and international appetite. Yet, prevention is possible, and the trend towards stricter standards and stronger partnerships suggests safer foodstuffs and healthier humans worldwide.
As former assistant FDA commissioner for Food Protection, Dr. David W. K. Acheson, notes in the June 10, 2012 issue of Food Safety News, “We are back to that old issue of controlling risk in the supply chain...it is not enough to focus on historical incidents...back to the farm is fast becoming the legal definition of responsibility.”
So, perhaps, in the interest of the preventive provisions of FSMA and other regulation, as well as a genuine desire to prevent outbreaks and promote public health, we will all – producers, distributors, suppliers, auditors, regulators and consumers – act more “responsibly,” and, while not growing, assessing, transporting or regulating our own food, will get to better know those who do.
Because, as Acheson emphasizes, “No matter where we call home, what language we speak, or culture or economy we follow, we are connected through the global marketplace, and that, as well as the implementation of the U.S. Food Safety Modernization Act, make it more critical than ever before that everyone – foreign and domestic – work together as partners in food safety.”
Read More:
Lead Article: Food Day Aims to Improve Diets, Strengthen Healthy Food Movement
CECHE News: CECHE Partners in D.C. and New Delhi to Boost Nutrition and Healthy Food Practices

Dr. Sushma Palmer, Program Director
Valeska Stupak, Editor & Design Consultant
Shiraz Mahyera, Systems Manager
Daniel Hollingsworth, Website Consultant