Center for Communications, Health and the Environment

India Faces New Health Challenges In 21st Century
by Sushma Palmer, D.Sc., Chairman, Center for Communications, Health & the Environment (CECHE), Washington, DC
India continues to suffer from consequences of poverty and underdevelopment, such as malnutrition and huge numbers of child and maternal deaths. However, major economic and social changes in recent decades have brought a new brand of health problems – non-communicable lifestyle diseases among the rich, the middle class and the poor.
By the year 2020, mortality from communicable, maternal and perinatal conditions, and nutritional deficiencies is expected to fall from almost 5 million to below 3 million a year in India, according to the 1996 Global Burden of Disease series issued jointly by the World Health Organization (WHO), the World Bank and the Harvard School of Public Health. At the same time, deaths from noncommunicable diseases (NCDs) and injuries in India are projected to almost double, from about 4 million to about 8 million a year (see accompanying article, “Global Health in Transition”). Thus, India faces new challenges in this century in confronting NCDs and their onslaught.
Modern Lifestyle and Food Patterns Are Increasing NCDs
India’s urban population has increased more than threefold in the last 40 years to more than 250 million, and the United Nations projects that by 2025, 50 percent of Indians will live in urban areas, a breeding ground for NCDs and their lifestyle-related triggers. Meanwhile, food patterns are changing. Even a decade ago, the urban middle class was estimated to consume only three-fourths the amount of cereals per capita compared to rural populations, and to derive more than 25 percent of calories from fats, oils, and milk and milk products; and the wealthiest urbanites were estimated to obtain up to 40 percent of calories from fats compared to 18.7 percent for rural adults, according to a 1998 report published in The Lancet. Although most Indians remain vegetarians, according to a 2003 WHO survey of 9,000 urban and rural Indian adults, fruit and vegetable intake fell below five servings/day in nearly 80 percent and below three servings/day in nearly 50 percent of those surveyed (see chart).
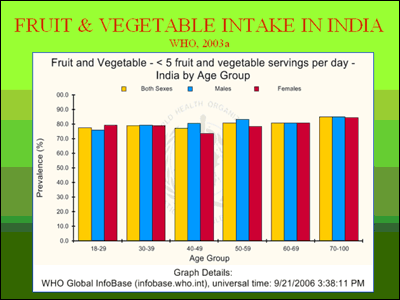
At the same time, physical activity and energy expenditure continue to decline, as more and more of India’s agricultural society evolves into industrialized communities. A 2003 WHO survey of more than 10,000 urban and rural Indian adults shows a high prevalence of physical inactivity, especially among middle-aged and older adults (see chart).

Such diets and lifestyle have exacerbated the incidence of abdominal obesity, insulin resistance, Type II diabetes, hypertension, cardiovascular disease and Syndrome X in India.
A survey of 11,000 urban adults in 2000 by A. Ramachandran and colleagues showed that 35 to 45 percent of middle-aged Indians had a body mass index (BMI) that exceeded 25 (see chart).
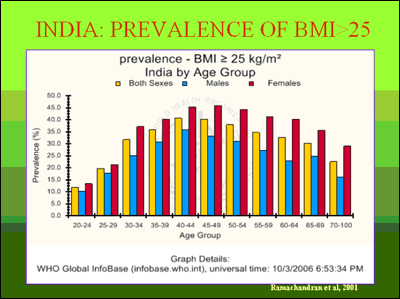
Previously, in 1998, Dr. C. Gopalan estimated the prevalence of abdominal obesity to be between 20 and 30 percent, projecting that it would double between 2002 and 2010 (see “Nutrition and Health Challenges” Q&A with Dr. Gopalan). As with obesity, Type II diabetes among middle-class adults and children in India is growing rapidly and is now six to 10 times more prevalent in India’s urban than its rural populations (see chart).
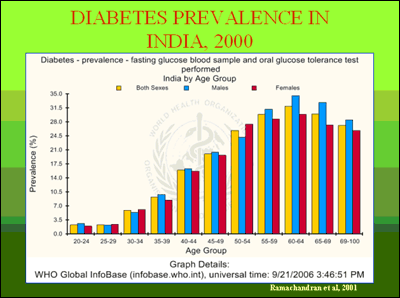
In short, India exemplifies the double jeopardy facing many developing countries and the challenges facing international and national policy-makers: halting escalating NCD epidemics worldwide, while confronting NCDs alongside infectious diseases, childhood and maternal mortality, and undernutrition in developing countries.
What Approaches Will Work Best for India?
So what can India do to reduce its risk of NCDs?
National nutrition policy in India encompasses a multifaceted approach, including chronic-disease prevention, but its overwhelming focus remains the prevention of childhood and maternal malnutrition and infectious diseases. Furthermore, it appears that the nation has yet to take full advantage of its television and other mass media to reach the masses. This is a missed opportunity.
The vast majority of Indians now have access to radio, and, even in villages, they view TV programs. In fact, television is the most effective medium for health communications, according to data collected during CECHE’s PSA Testing and Health Beliefs Program in 2000 in South India. Indians also love music. Thus, given India’s low literacy rates in several areas, visual media offer a special channel to mold public opinion on nutrition and health issues. The food industry is already using TV, radio and the print media to push fast foods; they know how to attract attention, and they are making significant headway.
One way that the Ministry of Health, Door Darshan and the health sector could outsmart the industry and advertising agencies is to beat them at their own game by using visual media effectively. This means outsourcing the production of public service announcements (PSAs), television series, musicals and ads to the very ad agencies that are producing them for the fast-food industry. The ads could feature major celebrities, Bollywood actors or sports heroes. They would need to lampoon bad eating habits and a couch-potato lifestyle; make it seem undesirable and costly in the long run to be obese; and bemoan lost years and quality of life, stressing that eating an unhealthy diet means getting sick, missing out on all the fun, dying early and not seeing your grandchildren grow up.
To succeed would require a massive and sustained national campaign, especially targeting children, because childhood is when food habits are formed. Such a campaign would need to be supported by training more health professionals and educators in public health and in the use of mass media for health promotion.
Initiatives like CECHE’s public health and nutrition scholarship program for master’s degree and doctoral candidates at Lady Irwin College in New Delhi exemplifies the strong motivation among nutrition students for such training (http://www.ceche.org/communications/lady-irwin/lady-irwin.html). Meanwhile, the nonprofit’s Media Training Program in India in 1998 demonstrated the advantages of joint training for health and media professionals in health promotion and disease prevention (http://www.ceche.org/communications/media1.htm).
A mass media approach has worked well for tobacco control in the United States and Australia. And CECHE’s experience in 1997 and 2000 in producing and testing PSAs in Punjab and South India tells us that it is likely to have a similar, positive impact in India, especially with support from the Nutrition Foundation of India, Lady Irwin College and other in-country organizations with health and nutrition expertise.
Considering the impact the print media has had in promoting diet and lifestyle in industrialized countries like the United States, India could also use more “objective” means of publicity to help compel the government and national lawmakers to develop policies and put programs into action. In addition, it would behoove the country to review, and on at least some level, incorporate, such major global health-promotion campaigns as “5-A-Day The Color Way,” which premiered in America and is now helping to encourage vegetable and fruit consumption across Europe via ads, PSAs and promotional materials targeting both children and adults.
Click here to read: Lead Article | Q&A | Companion Article

Dr. Sushma Palmer, Program Director
Valeska Stupak, Editorial & Design Consultant
Shiraz Mahyera, Systems Manager
Rohit Tote, Website Consultant